While breathing is often taken for granted, the responsibilities of caring for a loved one with pulmonary diseases like COPD can profoundly affect every breath they take and the lives of their caregivers. The CDC reports over 15 million Americans living with COPD, each supported by devoted loved ones facing unique challenges.
From work to spending time with friends to doing simple tasks like climbing stairs or walking the dog, many of the things we take for granted suddenly present a challenge. COPD can be psychologically exhausting too, increasing your loved one’s risk of serious health complications, including arthritis, asthma, congestive heart failure, diabetes, and stroke.
COPD Home Care
If your loved one has COPD, regular hospital stays and a severely limited quality of life often become the status quo. Many choose to manage the condition at home with their family since it’s a familiar place of love, comfort, and peace.
However, caring for COPD at home puts a heavy burden on the shoulders of the caregivers. Friends and family can and frequently do make huge sacrifices to keep life comfortable for loved ones with COPD. While noble, these sacrifices can come with significant personal, emotional, and physical demands. Caregiver burnout is dangerously real and puts both you and your loved one at risk.
Asking for help is essential when you’re caring for someone with COPD. And taking time to look after yourself can help you provide better care. This article breaks down how to cope with COPD as a family member, the ins and outs of providing home COPD care, and how to get the caregiver support you need.
Are you or a loved one living with a chronic or terminal illness?
The Sage Family of Companies is here to help.
Are you or a loved one living with achronic or terminal illness?
The Sage Family of Companies is here to help.
How to Spot COPD Symptoms
There’s a list of early warning signs that signal COPD, but this lung condition often isn’t diagnosed until its more severe stages.
Early warning signs
The main COPD symptoms during the earliest stages include:
- A cough that brings up a large amount of mucus and continues for a long time.
- Breathlessness, which may become more obvious after bouts of physical exertion.
- Chest heaviness, or a tight feeling in and around the chest area.
- A wheezing, whistling, or squeaky sound while breathing.
The above COPD symptoms may not all be noticeable at first, or the individual with COPD might make slight adjustments to compensate without realizing it. For example, a COPD patient may choose to drive short distances instead of walking.
If your loved one regularly coughs, gets lung infections, or has difficulty breathing, it’s a good idea to visit a physician early, to talk about COPD care or rule out other illnesses. Your family member’s doctor may refer them to a lung specialist, or pulmonologist, who will perform a basic test called spirometry. This test measures how much air the lungs expel in a single breath.
Severe COPD symptoms
As the disease advances, the following COPD symptoms can emerge:
- Anxiety
- Depression
- Fatigue
- Reduced appetite
- Unwanted or unexpected weight loss and muscle loss
Your loved ones with COPD may also discover that some previously easy activities become more difficult, often causing shortness of breath. Gardening or walking to the store, for instance, may cause unexpected panting and wheezing.
Recognizing COPD Flare-ups
Because COPD makes the lungs weaker, your loved one’s body will struggle to protect itself from smoke inhalation, colds, or lung infections. Even cold air and certain smells can trigger a flare-up.
When a person with COPD experiences a flare-up, it can cause:
- More extreme breathlessness than usual
- A tight chest
- Increased coughing
- Differently colored spittle
- Fever
The severity of a flare-up depends on the extent of the lung damage. Many severe flare-ups require in-hospital COPD care and treatment to control lung damage and improve symptoms. A flare-up becomes a medical emergency if:
- Your loved one struggles to talk or catch their breath.
- Their lips or fingernails have taken on a bluish tint.
- They show signs of confusion or delirium.
- They have a rapid heartbeat.
- The treatment they usually take isn’t having the intended effect.
Call 911 immediately if you notice these symptoms.
End-stage COPD Symptoms
While it’s possible to manage the more harmful effects of the condition, COPD doesn’t get better and eventually makes it difficult to function normally. Eventually, your family member with COPD will need 24-hour attention. Signs that you’ll need to consider end-of-life COPD care for your family member include:
- Difficulty walking, swallowing, and eating
- Regular lung infections
- Frequent, debilitating flare-ups
- Pain
- An increased number of hospital visits that require more days for each stay
- Increased anxiety and depression
- Muscle twitches and weakness
- Changes in breathing pattern and loudness
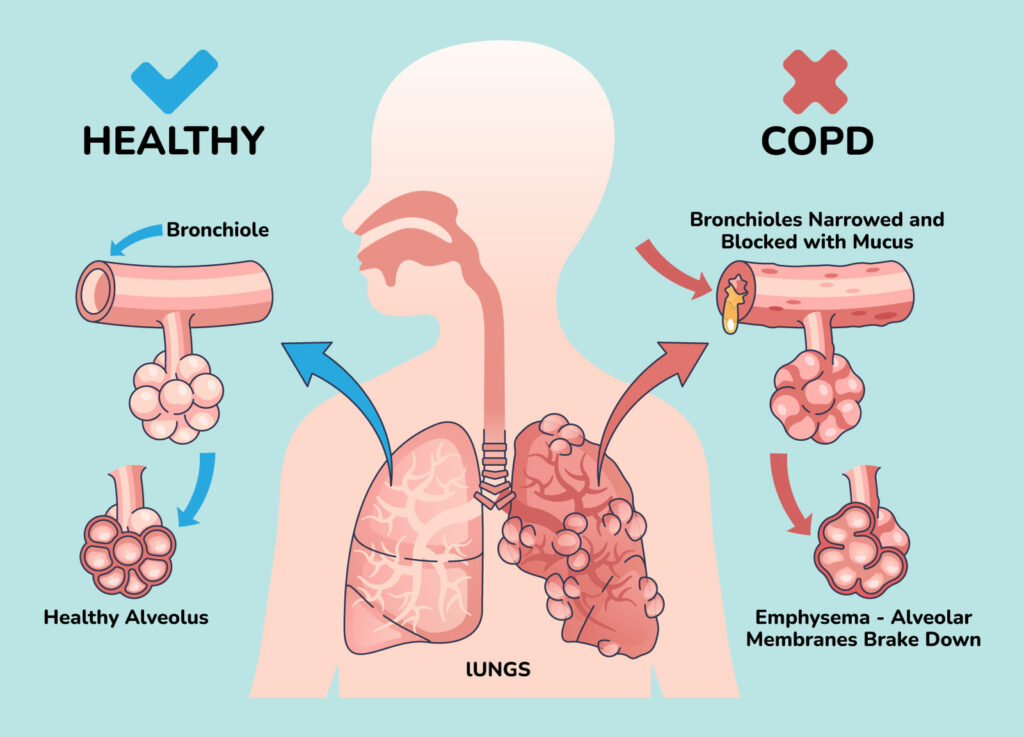
While your loved one may not die of COPD or low oxygen, the condition can cause heart complications like stroke and congestive heart failure, which are often fatal. As of 2022, COPD was the sixth leading cause of death in the United States. Once COPD starts causing these symptoms, the best COPD care you can provide is to support your loved one and provide relative comfort during their final days.
Are you or a loved one living with a chronic or terminal illness?
The Sage Family of Companies is here to help.
Are you or a loved one living with achronic or terminal illness?
The Sage Family of Companies is here to help.
How to Help Someone With COPD
Your loved one may not even know they have COPD at first. However, COPD is often progressive, and as symptoms become more disruptive, the responsibility you shoulder as a COPD home caregiver will increase dramatically.
Dealing With COPD at Home
There are certain measures caregivers in the family can take to create a safe environment for someone with COPD. The measures below can make your loved one’s life as comfortable as possible.
- Attending doctor’s appointments with your loved one and taking notes on the physician’s advice.
- Tracking your loved one’s medication and oxygen schedule on your phone so you can support the treatment regimen and track when to refill prescriptions.
- Pitching in with errands and household chores your loved one may not have the energy to tackle.
- Engaging your loved one in a light exercise routine during COPD care to maintain lung health.
- Providing support during periods of depression and stimulation when your loved one cannot leave the house. Consider doing simple things with them, like playing a card game or watching their favorite movie. Even talking can help them feel less isolated.
- Consider professional help that can ease the pressure on your family while providing pain relief and improving your loved one’s quality of life. Sage Hospice provides personalized care plans administered by highly experienced palliative and hospice care nurses to help COPD patients live comfortable, fulfilled lives with their condition.
Home Safety During COPD
When you’re caring for COPD patients, it’s important to account for their reduced ability to expend energy and help them around the home. Maintaining clean air is important too, to prevent flare-ups and keep symptoms at a manageable stage as long as possible.
- Set up a ground-floor living space. This reduces or eliminates your loved one’s need to climb the stairs.
- Replace any carpeted floors with hardwood or tile flooring. Carpet can build up dust or pollutants like pet dander, risking flare-ups during COPD care. Not everyone can simply rip up carpets, though, so it can help to use a vacuum with a HEPA filter regularly. You can also steam-clean furniture, carpets, and curtains every six months.
- Ban smoking in the home. Preventing exposure to tobacco smoke will support your family member’s journey toward quitting and protect them from harmful second-hand smoke exposure.
- Install an air purifier. This can reduce pollutants in the environment, especially if the purifier has a HEPA filter.
- Choose natural, non-toxic cleaning and air freshening products. Many cleaning products contain harsh chemicals, and using these can risk a flare-up.
- Book an air duct and AC inspection. This often-neglected aspect of home safety becomes essential while caring for COPD patients, as clean airflow is central to managing symptoms.
- Prepare the bathroom. The bathroom presents a risk of slips and falls during periods of low energy. It also traps moist air that can trigger flare-ups. Using a shower chair can help COPD patients conserve energy. It’s also important to make sure the room is well-ventilated by opening the window, showering with the door open, or using an exhaust fan.
- Purchase a portable oxygen tank. This allows your loved one to keep up with supplementary oxygen while retaining some measure of mobility and freedom during COPD care.
Communicating With Someone You Love Who Has COPD
Knowing how to deal with COPD as a family member can be especially difficult because it’s so emotionally draining. Those living with COPD often feel a constant sense of depression, anger, and guilt, and talking can become physically difficult. While caring for COPD in a loved one, you’ll often have to calm your family member and steer them through an increasing loss of independence and self-esteem.
- Don’t assign blame. As a smoking-related condition, a “blame culture” surrounds COPD, and your loved one is likely to feel shame. Though you may feel some anger too, it’s important not to let this spill over into your conversations with your family member.
- If they’re finding it too hard to talk, encourage them to write you letters or electronic messages, even if you live together. Knowing they don’t have to exert themselves by talking may help your loved one open up.
- Help them find a support group if they feel uncomfortable discussing certain aspects of the disease. A group that supports video group calls can help them connect without the risk of breathlessness that can accompany leaving the house.
- Accept that your loved one with COPD may feel more comfortable sharing their thoughts with someone outside the family like a friend, counselor, religious leader, or advice line.
Support for Caretakers of COPD: How to Look After Yourself During COPD Care
Caring for COPD patients can take a toll on the caretakers. It requires intensive and often costly work around the home, like removing carpets. The caretaking process can be time-consuming during severe COPD or flare-ups.
Caregiver burnout is a very real concern during these times, as it can become easy to prioritize your loved one’s needs over your own health and well-being. However, it’s crucial to look after yourself while you’re looking after the one you love. Care is tough, round-the-clock work, and being constantly drained and overtaxed is also harmful to your health.
The following measures can help you avoid burnout during care:
- Take regular breaks to do something that nourishes you, and avoid losing sight of the activities you enjoy. This can be easier said than done, but it’s important for your health.
- Talk to friends, family, or mental health professionals about the impact of caretaking.
- Engage in mindful relaxation, like deep breathing, yoga, meditation, or taking a long, hot bath.
- Make sure you eat and sleep enough, and take time to prepare your favorite meal. This will help you stay fed and give you a boost of much-needed happiness.
- Join a COPD care support group to speak to other caretakers.
- Seek permission from your loved one with COPD to introduce friends and other family members to the caregiving process. Many hands can make for lighter work.
- Don’t shy away from asking your loved one’s medical team for advice. Caring for COPD patients
Support for Caretakers of COPD
It’s possible to reduce the risk of COPD flare-ups in a tightly controlled environment, but COPD doesn’t get better. Over time, symptoms will become more severe and flare-ups more frequent. Needing help with your loved one isn’t an admission of defeat. It’s a sign that it’s time for professionals to step in, relieve your burden, and restore comfort to your family member’s life.
If you’re consistently tired and stressed or you’re at the peak of caregiver burnout, respite care can become a central aspect of caring for your loved one — and for yourself. Care professionals can ease the pressure on you without missing a beat in the treatment plan, freeing you up to manage your life, run errands, attend personal engagements, and relax.
How Home Support can Help COPD Caregivers
Professional home COPD caregiver support can include help with chores and errands, socialization and company, and ensuring comfort for your loved one. Some COPD patients will only need a few hours of care a day, while more advanced COPD symptoms might need 24-hour care.
Flexible, in-home respite care can support practical needs like dressing, bathing, food prep, and light housework. When caring for COPD patients requires full-time bedside care and monitoring, a professional home-care aid can provide relief for patients and caregivers alike.
Palliative and Hospice Care for COPD
Accepting the idea of palliative and hospice care can be tough for everyone, but it’s essential to make plans while your loved one is still well enough to make decisions about their own healthcare journey. Talking about this kind of care can be painful and difficult, but whether your loved one enters in-hospital or at-home palliative and hospice care, the ultimate goal is to improve the comfort of those living with COPD.
Palliative Care
People at any stage of COPD can benefit from receiving palliative care. A dedicated medical team consisting of specialists, nurses, and social workers can provide medical, social, and mental health support for those isolated by COPD. These kinds of COPD care services provide pain relief and aim to preserve the patient’s quality of life. They can also improve comfort at any stage of the disease, even while the patient is still undergoing treatment.
Sage Family of Companies’ palliative care services provide personalized, empathetic palliative care that prioritizes emotional and physical comfort for your loved one.
Hospice Care
Your loved one’s passing is never easy to think about while you’re caring for COPD. Keep in mind that hospice care can support comfort, peace, and dignity during their last days. A specialized team of doctors, nurses, grief counselors, massage therapists, and spiritual advisers can provide pain relief, ease your loved one’s passing, and ensure that their religious, spiritual, and emotional needs are met.
Sage Family of Companies hospice care can be a source of calm and assurance in the final, painful stages of COPD, either at home or in a dedicated facility. Our hospice nurses are trained and equipped to provide medical support and compassion during a difficult time, letting you tend to the many arrangements that accompany the end of life. With help from one of the Sage Family of Companies hospices, you can take your own time to protect your emotional health.
COPD Care: The Bottom Line
COPD overturns lives, increases pain, and brings with it a level of guilt and anger that can make communication difficult. Asking for help can feel like giving up, but it’s actually the next step in taking better care of your loved one and their condition while supporting their caregivers.
Your family understandably expects you to be there for them, but they don’t expect you to have infinite stamina. If you burn out, your ability to offer effective care will suffer. Respite care is there for you if your loved one’s COPD becomes severe, if there are too many flare-ups, or if you simply find yourself unable to cope.
Whether you seek support from your family and friends or you go the professional route, don’t carry the burden alone. Before and during your loved one’s final chapter, make one of the Sage Family of Companies your choice for COPD care. You don’t have to go through this on your own.
The Sage Family of Companies is here to answer any questions you may have.
Article resources:
- Booker, R. (2005). Effective communication with the patient
- Chronic Obstructive Pulmonary Disorder. (2021)
- COPD symptoms. (2022)
- Difficult conversations – tips from people who are living with COPD. (n.d.)
- Finding the COPD support you need. (n.d.)
- Leading causes of death. (2022)
- Living with COPD. (n.d.)
- What are the physical signs in the last weeks or days? (2021)